Origin: Mesodermal.
The male reproductive system
Consists of :
•primary sex organs (a pair of testes),
• secondary sex organs ( duct system and associated glands)
• External genitalia(penis and scrotum).
The
duct system includes Epididymis, vas deferens, ejaculatory ducts
and urethra.
The associated glands are seminal vesicles, prostate gland and cowper's gland.
•Testes and scrotum: testes are primary sex organs and responsible
for production of gametes and sex hormones.
A pair , lies inside scrotal Sac
which are extra abdominal,
out pocketed Sac like Structure.
Inside testis, formation, maturation and storage of sperms take place and for
it low temperature about (2- 2.5)°C less than body temperature is required.
Thus, testis are extra abdominal.
In Chitopteras(Bats),
Cetaceans(aquatic mammals), proboscideas(elephants) and Prototherians(egg
laying mammals) , intra abdominal testis are present.
The scrotal sac is Sac of Skin ,
is highly pigmented and rich in sweat glands. It Contains Dartos muscle. It is
homologous to Labia majora of female.
Testis remains Connected with
abdominal Cavity by spermatic Cord which passes through inguinal Canal. The
spermatic Cord Consists of blood vessels, lymph vessel, nerve, vas deferens and
Cremaster muscle.
The dartos muscle and cremaster
muscle are smooth muscle and Sensative to temperature. They Contract When
temperature is low and scrotal sac along with testis ascends while relaxes when
temperature is high and scrotal sac along with testis descends.
The scrotal sac remains
differentiated into 2 Parts by scrotal septum. Inside each scrotal sac , a
testis is present.
The left testis is slightly lower than right testis.
Development: After fertilization about (7-8) week development of testis begins in abdominal Cavity just below kidney. At about (7-8) months of development , they start to descend and they move inside scrotal sac through inguinal Canal which connects abdominal Cavity and scrotal sac.
• Cryptorchidism: Testes not present in scrotal sac. This is due to
failure of one or both testis to descend into scrotal sac.
• orchidoplexy: surgical process to Correct cryptorchidism.Testis remains attached with scrotal sac at lower end by Gubernaculum.Each testis is Small, oval, pink coloured structure of (4-5) cm length (2-3) cm width and 3cm thickness.
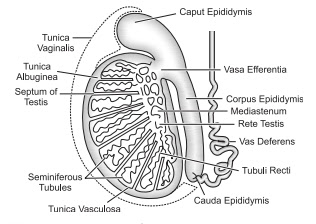
protection: just outside 3 layers are present which are,
•Tunica vaginalis: outer and incomplete layer. It has outer layer
and inner layer. sometimes serous fluid get deposited in between these layers
and it is called hydrocoeI.
• Tunica albuginea: is middle fibrous layer.
• Tanica vasculosa: Inner thin layer, rich in blood capillaries.
The tunica albuginea extends
inward and forms a number of testicular lobules about (200-300). Each
testicular lobule contains about (1-4) highly coiled seminiferous tubules. Thus
, about 750 seminiferous tubules are present inside each testis. Each
seminiferous tubule remains lined by two type of cells; male germ cells and
sertoli cells. The male germ cells
undergo process of spermatogenesis to form sperm.
The Sertoli Cells or Nurse cells or sustentacular cells provide
nutrients to germ Cells and developing spermatogonia. It is Phagocytic in nature and Cause
phagocytosis of worn out cells. It forms blood testis barrier (to decrease
temperature of testis). They are stimulated by FSH. They produce ABP, Inhibin
and AMF.
• ABP_ Androgen binding protein: Binds with androgen
(testosterone) and keeps
testosterone inside seminiferous tubules.
• Inhibin: Has inhibitory effect on pituitary /hypothalamus for the
production of FSH and LH.
• AMF- Antimullerian factor: Inhibits the development of feminine
Characters in male.
The region outside Seminiferous tubules, the interstitial space Contains small blood vessels and interstitial Cells or Leydig's Cells which are endocrine in nature and influenced by LH. They produce male sex hormone testosterone which is responsible for the development of secondary sex Characters and spermatogenesis. The testosterone enter inside seminiferous tubules and stimulate germ cells for spermatogenesis.
Hormonal mechanism:
Hypothalamus ⇒ GnRH → pituitary → FSH(stimulates
sertoli cell) & LH(stimulates Leydig’s cell).
• Castration: Surgical or Chemical removal of testicles. surgical
removal of testis is Called Orchidectomy.
Castration of male animals is done
to Control behaviour and increase fat production.
Testosterone increases aggression.
eg. Ox.
Bull → Aggressive.
ox → Docile.
It is also responsible for the development
of secondary sex Characters and
spermatogenesis. The testosterone enter inside seminiferous tubules and
stimulate germ cells for spermatogenesis.
The Seminiferous tubules end into short and straight tubular structure Called tubuli recti which leads into network of fine tubules called rete testis. From rete testis, about (10- 12) fine ducts called Vasa efferentia arises and they open into epididymis.
The tubuli recti, rete testis
& vasa efferentia are present inside testis. so, they form intratesticular
duct system.
• secondary sex organs: Those organs which are not
directly involved in gamete production. They are involved in storage,
transportation and maturation of gametes are secondary sex organs. These are:
Epididymis, vas deferens,
seminal vesicles , prostate
glands, Cowper's gland and penis.
• Epididymis: long and highly coiled tubular structure of about (6
-7) m in length. It is found on external surface of testis. It has 3 parts:
• Caput epididymis: It is
upper or head part and the vasa
efferentia opens into it.
• Corpus Epididymis: It is
main body part.
• Cauda Epididymis : - The
Posterior part or tail. It Connects epididymis to vas deferens.
It is site for temporary storage, maturity and mobility of spermatozoa. The pattern of mobility and percentage of mobility changes from Caput epididymis to Cauda epididymis. The spermatozoa Can remain alive for about one month in Cauda epididymis. Though sperm acquire mobility in epididymis yet they don't move on their own. They are propelled by fluid movement. once they are ejaculated in female reproductive tract they get capacitation and survive for about 72 hrs.
Epididymis also nourishes
spermatozoa.
Epididymis and testis are Collectively Called testicle.
• Vas deferens or Ductus deferens: Cauda epididymis leads into vas deferens. It is about 45cm long and ascends along the posterior border of epididymis through spermatic Cord and enters into abdominal Cavity where it loops over the ureter of own side and passed down the posterior surface of Urinary bladder. At terminal end get dilated to form ampulla where sperm is stored for sometime (secondary storehouse). It receives duct from seminal vesicles and becomes ejaculatory duct which opens into urethra.
It's function is to Carry sperms during sexual arousal from epididymis towards urethra by peristaltic movement. The sperms that are not ejaculated by that time are reabsorbed.
• seminal vesicles: 1 Pair
, convoluted Pouch like structures of about 5 cm length and lies Posterior to
urinary bladder and anterior to rectum.
They are glandular in nature and
secrete alkaline, viscous fluid that Contains fructose, prostaglandins and
clotting factors.
The alkaline nature of Seminal
fluid helps to neutralise the acidic nature of male urethra and female
reproductive tract.
• Fructose provides nutrients to sperm.
• prostaglandins is responsible
for sperm mobility and viability. It stimulates Contraction of smooth muscles
of female reproductive tract for the movement of sperms.
• The Clotting factors help Semen
to coagulate after ejaculation as Cannot Survive in acidic vagina. Thus, live
in clot & alkaline medium.
The seminal fluid forms about
(60-70)% part of semen.
•Prostate gland: It is
single doughnut Shaped gland about the size of golf ball. It is inferior to the
urinary bladder and surrounds the prostatic part of urethra. The Prostate
slowly increases In size from birth to puberty. It then expands rapidly until
about the age of 30, after which it's size remains stable up to age 45, then
further enlargement may occur.
• BPH: Benign Prostatic
Hyperplasia: Enlargement of prostate gland in advanced age. It Compresses
urethra and Urination become Painful and difficult.
• Surgical removal of prostate
gland is Called prostatectomy.
• The prostate gland produces
prostatic fluid which is milky and slightly acidic ( PH about 6.5). It Contains
Citric acid (used as nutrients by sperms) , enzymes like prostate specific
antigen , lysozyme, amylase, hyaluronidase ( breaks
down clotting protein from seminal vesicle)
The seminalplasmin in Prostatic fluid is antibiotic and kills naturally
occuring bacteria in semen and in lower female reproductive tract.
The prostatic Secretion make about
(20-25)% part of semen and is responsible for sperm mobility and viability.
• Cowoper's gland ( Bulbourethral gland): A pair of small pea sized gland on either side of
membranous urethra and their ducts open into membranous urethra. During sexual
arousal they secrete alkaline fluid which neutralises acidic nature of urethra
due to urine. They also produce mucus which lubricates the end of penis and
lining of urethra.
• penis or Male Copulatory organ: It is cylindrical, erectile, spongy and consists of body,
glans penis and root.
• The body of penis consists of
three Cylindrical masses of tissue each surrounded by fibrous tissue Called tunica
albuginea. Two dorsolateral masses are Called Corpora cavernosa while smaller midventral mass is Called Corpus spongiosum with penile urethra.
skin and a subcutaneous layer
enclose all three masses. These Cylindrical masses Contain erectile tissue
which is composed of numerous blood
sinuses surrounded by smooth muscles and elastic connective tissue.
The distal end of Corpus
spongiosum is enlarged and Called glans penis which is highly sensative(as many
many nerve endings are present here). It remains covered by a thin fold of
refractile Skin Called foreskin or prepuce. surgical removal of prepuce is
Called circumcision. Urethra opens at the top of glans penis by urethral
orifice.
The prepuce internally Contains
prepuceal gland or gland of Tyson which produces white creamy substance called
smegma which is Carcinogenic.
The penis is male Copulatory organ and urine & semen passes out through it.
• Ejaculation: The release of semen from urethra during sexual intercourse is Called ejaculation which is sympathetic reflex.
During it, the internal urethral
Sphincter closes urinary bladder to prevent expell of urine from urinary
bladder and entry of sperms into bladder.
The erection of penis is due to
the Parasympathetic nerves while ejaculation is due to sympathetic nerves.
The inability of penis to achieve
successful erection is Called erectile dysfunction or Impotence. viagra (
sildenafil Citrate) is used to Correct it.
• Semen: It is mixture of sperms ( 10 / %), seminal fluid ( 60- 70 )%, prostatic fluid (20-25)% and secretion of Cowper's gland (<1)%. The volume of semen in a typical ejaculation is about (2.5- 3.5)ml ( about 3ml) with about 200 to 300 million (about 100 million per ml ) sperms. At least 60% sperms must have normal shape and size and 40% of them must show vigorous mobility.
☆ Introduction of semen into
female reproductive tract is called insemination.
☆ The process by which sperm gets
Capacity to fertilize ovum is called Capacitation. It occurs in female
reproductive tract (fallopian tube).
☆
Movement of sperm: sperm→
seminiferous tubules → tubuli recti → Rete testis → vasa efferentia →
Epididymis → vas deferens → Ejaculatory duct → urethra → urethral orifice →
out.
☆ Ligation (Cut & tie) of vas
deferens is Called vasectomy which
is permanent method of family planning for male.
☆ Azoospermia: NO sperm Count.
☆ Oligospermia:
sperm Count <15 million per ml of Semen.
☆ Male seminal fluid Contains Fructose, which is a forensic indicator of rape as is not produced elsewhere in body.